Periodontal Disease
Periodontal
disease, or gum disease, is a general term that refers to a bacterial infection
of the tissues that support the teeth. These tissues include: the gums, the
bones that surround the teeth, and the fibers that attach the teeth to the gums
and bone. The two types of periodontal
disease are gingivitis and periodontitis.
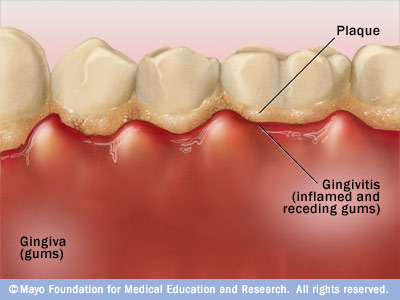
Gingivitis is a bacterial infection that damages the gums and causes them to become red, swollen, sensitive, and prone to bleeding. Fortunately, gingivitis is reversible if regular dental visits, brushing, and flossing resumes. Periodontitis is also a bacterial infection that damages the gums, however it also damages the bone that surrounds teeth and the attachment fibers. Unfortunately, the damage caused by periodontitis is not entirely reversible.
Periodontal disease begins with the build-up of a sticky film that contains bacteria, called plaque, on the teeth. When teeth are not cleaned regularly, this sticky film adheres to teeth and allows layers of bacteria to build up on the teeth and gums; this bacteria results in higher levels of acid in the saliva which causes damage to the tissues. Our body detects this bacteria and begins to mount an immune response, which if prolonged can cause even more damage to the gums.
If this plaque is not regularly removed, then gingivitis occurs. As previously mentioned, in gingivitis the gums become damaged and may become swollen, red, and can bleed during brushing and flossing. Gingivitis may last anywhere from a few weeks to years. If this gingivitis is not caught and treated, there is a possibility that it may progress to periodontitis.
Periodontitis may become aggressive, which results in rapid bone loss, or chronic which progresses more slowly; however both types should be treated immediately. With more frequent dental cleanings with specialized treatment, brushing, and flossing the periodontitis may be stopped before it can cause a great deal of damage. However, if not treated the periodontitis continues to cause damage to the gums and bone surrounding the teeth; eventually this reduction of bone can lead to teeth being lost. With periodontitis, the more obvious signs of bleeding, swelling, and redness may not be present and can be mistaken for health. The progression of periodontal disease can be accelerated by the presence of local and systemic contributing factors.
Local contributing factors are conditions in the mouth that can contribute to a person’s susceptibility to periodontal disease. Some examples of these factors include: calculus (which is sometimes called “tartar”), cavities, rough edges of some fillings or crowns, and sometimes the natural ridges or grooves of a tooth. These factors encourage the plaque to build up on the teeth or can allow bacteria that are more capable of causing periodontal disease to thrive.
Systemic factors are conditions or diseases that involve the major systems of the body and can increase someone’s susceptibility to disease, usually by changing the way the person’s body reacts to disease-causing germs. One of the major systemic factors that increase a person’s likelihood of developing periodontal disease is smoking; smoking makes a person more likely to acquire periodontal disease, more likely to have severe bone loss and damage to the oral tissues, and causes delayed wound healing. Diabetes can also increase the chances of having periodontal disease, unless it is well-controlled. There are many other possible systemic factors including: osteoporosis, hormonal changes, Down syndrome, leukemia, and AIDS. Even some medications can have side effects that can contribute to periodontal disease.
Gingivitis is a bacterial infection that damages the gums and causes them to become red, swollen, sensitive, and prone to bleeding. Fortunately, gingivitis is reversible if regular dental visits, brushing, and flossing resumes. Periodontitis is also a bacterial infection that damages the gums, however it also damages the bone that surrounds teeth and the attachment fibers. Unfortunately, the damage caused by periodontitis is not entirely reversible.
Periodontal disease begins with the build-up of a sticky film that contains bacteria, called plaque, on the teeth. When teeth are not cleaned regularly, this sticky film adheres to teeth and allows layers of bacteria to build up on the teeth and gums; this bacteria results in higher levels of acid in the saliva which causes damage to the tissues. Our body detects this bacteria and begins to mount an immune response, which if prolonged can cause even more damage to the gums.
If this plaque is not regularly removed, then gingivitis occurs. As previously mentioned, in gingivitis the gums become damaged and may become swollen, red, and can bleed during brushing and flossing. Gingivitis may last anywhere from a few weeks to years. If this gingivitis is not caught and treated, there is a possibility that it may progress to periodontitis.
Periodontitis may become aggressive, which results in rapid bone loss, or chronic which progresses more slowly; however both types should be treated immediately. With more frequent dental cleanings with specialized treatment, brushing, and flossing the periodontitis may be stopped before it can cause a great deal of damage. However, if not treated the periodontitis continues to cause damage to the gums and bone surrounding the teeth; eventually this reduction of bone can lead to teeth being lost. With periodontitis, the more obvious signs of bleeding, swelling, and redness may not be present and can be mistaken for health. The progression of periodontal disease can be accelerated by the presence of local and systemic contributing factors.
Local contributing factors are conditions in the mouth that can contribute to a person’s susceptibility to periodontal disease. Some examples of these factors include: calculus (which is sometimes called “tartar”), cavities, rough edges of some fillings or crowns, and sometimes the natural ridges or grooves of a tooth. These factors encourage the plaque to build up on the teeth or can allow bacteria that are more capable of causing periodontal disease to thrive.
Systemic factors are conditions or diseases that involve the major systems of the body and can increase someone’s susceptibility to disease, usually by changing the way the person’s body reacts to disease-causing germs. One of the major systemic factors that increase a person’s likelihood of developing periodontal disease is smoking; smoking makes a person more likely to acquire periodontal disease, more likely to have severe bone loss and damage to the oral tissues, and causes delayed wound healing. Diabetes can also increase the chances of having periodontal disease, unless it is well-controlled. There are many other possible systemic factors including: osteoporosis, hormonal changes, Down syndrome, leukemia, and AIDS. Even some medications can have side effects that can contribute to periodontal disease.
- Frequently
Asked Questions?
A: Bacteria in plaque is what initiates the periodontal disease, however it is the body’s immune response and inflammation that causes the majority of the damage to the gums and bone.
Q: Once I have periodontitis will I have to worry about it for the rest of my life?
A: Yes, unfortunately you will always be more prone to periodontal disease and will need to be vigilant with bruhing and flossing. Usually, you will also need to schedule more frequent dental hygiene appointments and specialized treatments.
Q: Once I have developed damage from periodontitis can my gums and bone ever return to a healthy state?
A: With dedicated care and regular dental treatment, you will see improved health of your gums (less bleeding and redness). However, once the bone is lost it cannot be naturally regained.
References
Dentalcare.com. (2014). What is Gum Disease?. Retrieved February 13, 2014 from http://www.dentalcare.com/en-US/dental-education/patient-education/periodon-english.aspx
Nield-Gehrig, J.S., & Willmann, D. (2011). Foundations of Periodontics for the Dental Hygienist (3rd ed.). Philadelphia: Lippincott Williams & Wilkins
(2014). Gingivitis. [Illustration]. Retrieved from http://www.mayoclinic.org/condition/gingivitis/multimedia/gingivitis/IMG-20006944
Dentalcare.com. (2014). What is Gum Disease?. Retrieved February 13, 2014 from http://www.dentalcare.com/en-US/dental-education/patient-education/periodon-english.aspx
Nield-Gehrig, J.S., & Willmann, D. (2011). Foundations of Periodontics for the Dental Hygienist (3rd ed.). Philadelphia: Lippincott Williams & Wilkins
(2014). Gingivitis. [Illustration]. Retrieved from http://www.mayoclinic.org/condition/gingivitis/multimedia/gingivitis/IMG-20006944